
HEALTH NEWS
Eczema and Food Allergies: Exploring the Connection
-
Rahul Priydarss
Understanding the link between eczema and food allergies is essential for effective management. While food allergies don’t directly cause eczema, they can exacerbate symptoms due to shared inflammatory pathways. Identification of trigger foods through methods like elimination diets or allergy testing is crucial. Lifestyle modifications, including moisturizing routines and stress management, complement dietary interventions in holistic eczema management. Consulting healthcare professionals ensures personalized treatment plans for individuals navigating these complexities.
What is Eczema:
Eczema, or atopic dermatitis, poses a persistent challenge due to its chronic nature and diverse triggers. Among these triggers, the association with food allergies has gained significant attention. Research indicates a considerable overlap, with many eczema sufferers also experiencing food sensitivities or allergies.
Eczema:
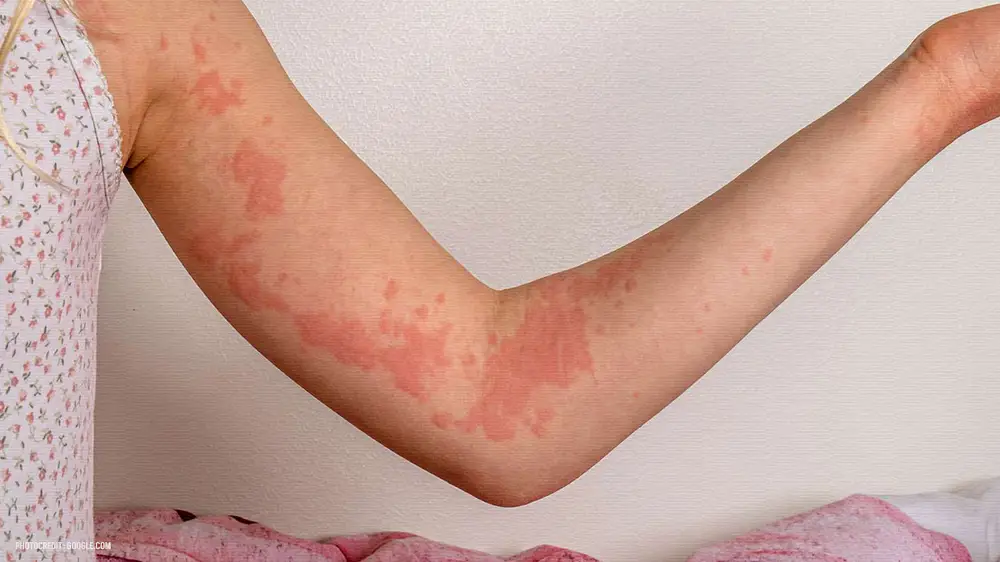
- Chronic inflammatory skin condition causing dryness, itchiness, and irritation.
- Appears as red, scaly patches on the skin.
- Most common type: Atopic dermatitis (often genetic and environmental).
- Other types: Contact dermatitis (irritants/allergens), Dyshidrotic eczema (blisters on palms/soles), Seborrheic dermatitis (scaly patches on scalp/face).
What is Food Allergies:
Food allergies are immune system reactions triggered by consuming certain foods. When someone with a food allergy ingests or comes into contact with a specific food allergen, their immune system mistakenly identifies it as harmful and produces antibodies to fight it off. This immune response can lead to various symptoms, ranging from mild to severe, depending on the individual’s sensitivity to the allergen.
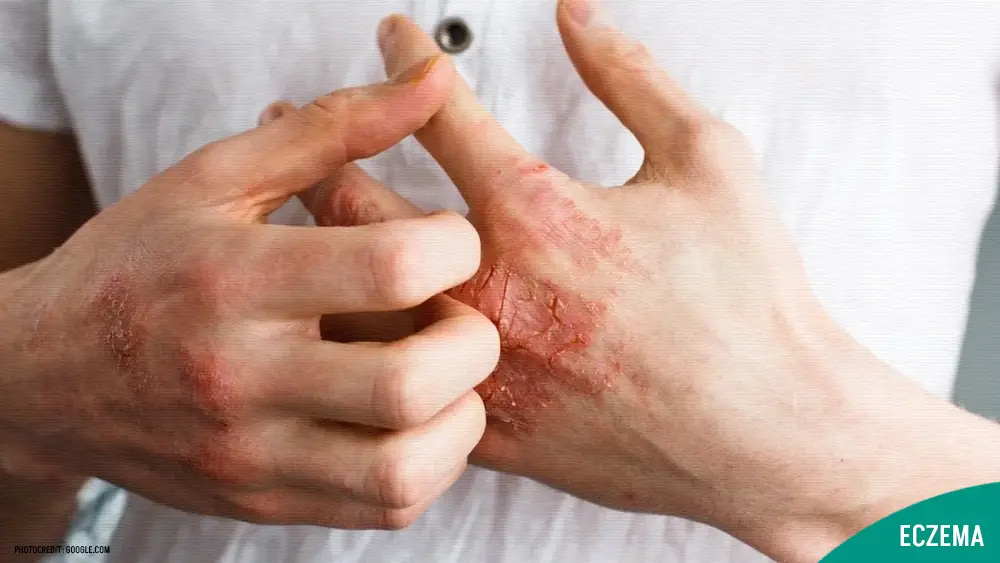
Table of Contents
Food Allergies:
- Immune system overreaction to specific foods.
- Symptoms can include hives, swelling, nausea, difficulty breathing (severe cases).
- Common triggers: Dairy, eggs, peanuts, tree nuts, soy, wheat, shellfish.
Why do food allergies cause eczema:
Actually, food allergies don’t directly cause eczema. Eczema is a chronic inflammatory skin condition with complex causes involving genetics and environmental factors. However, food allergies can worsen existing eczema symptoms and trigger flare-ups in some individuals. Here’s why.
Inflammation Connection: Both eczema and food allergies involve inflammation in the body. When a food allergy is triggered, the immune system overreacts, leading to inflammation throughout the body. This can worsen the existing inflammation in the skin, intensifying eczema symptoms.
Leaky Gut Theory: This theory suggests that in some eczema patients, the gut lining may be compromised. This allows undigested food particles (including potential allergens) to enter the bloodstream more easily. The immune system can then react to these particles, triggering an inflammatory response that can manifest in the skin as worsened eczema.
Link Between Eczema and Food Allergies:
The link between eczema and food allergies is complex and not fully understood, but there is evidence to suggest that food allergies can play a role in triggering or exacerbating eczema symptoms in some individuals. Here are some key points about the relationship between eczema and food allergies.
Increased Prevalence: Individuals with eczema are more likely to have food allergies compared to the general population. Studies have shown that up to one-third of children with moderate to severe eczema also have food allergies.
Early Onset: Food allergies and eczema often develop in infancy and early childhood. Babies with eczema are at higher risk of developing food allergies, and early exposure to potential allergens may increase this risk.
Biological Mechanisms: The exact mechanisms linking eczema and food allergies are not fully understood but may involve disruptions in the skin barrier function and immune system. In individuals with eczema, the skin barrier is compromised, making it easier for allergens to penetrate the skin and trigger immune responses.
Food Triggers: Certain foods are more commonly associated with triggering eczema flare-ups in susceptible individuals. Common food allergens such as cow’s milk, eggs, peanuts, tree nuts, wheat, and soy are known to exacerbate eczema symptoms in some people.
Atopic March: The progression of allergic diseases from eczema to other allergic conditions, such as asthma and allergic rhinitis, is known as the “atopic march.” Food allergies may play a role in this progression, as children with eczema and food allergies are more likely to develop asthma and other allergic conditions later in life.
Identification and Management: Identifying and managing food allergies can be challenging but is essential for controlling eczema symptoms. Allergy testing, such as skin prick tests or blood tests, can help identify specific food allergens. Once trigger foods are identified, avoiding them in the diet can help reduce eczema flare-ups.
Individual Variability: It’s important to note that not all individuals with eczema have food allergies, and not all food allergies lead to eczema. Eczema triggers can vary widely from person to person, and food allergies may only be one contributing factor among many.
Types of Eczema:
Eczema, or atopic dermatitis, encompasses several types, each with its own distinct characteristics and triggers. The most common types of eczema include.
Atopic Dermatitis: This is the most common form of eczema, typically appearing in childhood and often persisting into adulthood. It is characterized by dry, itchy skin and may be accompanied by redness, inflammation, and thickened patches of skin. Atopic dermatitis is associated with a family history of eczema, asthma, or allergic rhinitis.
Contact Dermatitis: Contact dermatitis occurs when the skin comes into contact with an irritant or allergen, leading to inflammation and a rash. Irritant contact dermatitis is caused by exposure to substances such as soaps, detergents, or chemicals, while allergic contact dermatitis is triggered by an allergic reaction to a specific substance, such as latex or nickel.
Dyshidrotic Eczema: Dyshidrotic eczema, also known as pompholyx, typically affects the hands and feet. It is characterized by small, fluid-filled blisters that cause itching, redness, and peeling. The exact cause of dyshidrotic eczema is unknown, but it may be associated with factors such as stress, allergies, or exposure to certain metals.
Seborrheic Dermatitis: Seborrheic dermatitis primarily affects the scalp, face, and other areas rich in oil glands. It is characterized by redness, greasy or scaly patches of skin, and dandruff-like flakes. Seborrheic dermatitis may be exacerbated by factors such as hormonal changes, stress, or certain medical conditions.
Nummular Eczema: Nummular eczema, also known as discoid eczema, appears as coin-shaped patches of inflamed, itchy skin. These patches may ooze, crust over, or become dry and scaly. Nummular eczema is often triggered by factors such as dry skin, irritants, or allergic reactions.
Neurodermatitis: Neurodermatitis, also known as lichen simplex chronicus, is characterized by thickened, leathery patches of skin that result from repeated scratching or rubbing. It often occurs in localized areas, such as the back of the neck, wrists, or ankles. Neurodermatitis is associated with psychological factors, such as stress or anxiety, which can exacerbate itching and scratching.
Stasis Dermatitis: Stasis dermatitis develops in areas of poor circulation, typically the lower legs and ankles. It is characterized by swollen, itchy skin, redness, and the formation of ulcers or sores. Stasis dermatitis is commonly seen in individuals with venous insufficiency or other circulatory disorders.
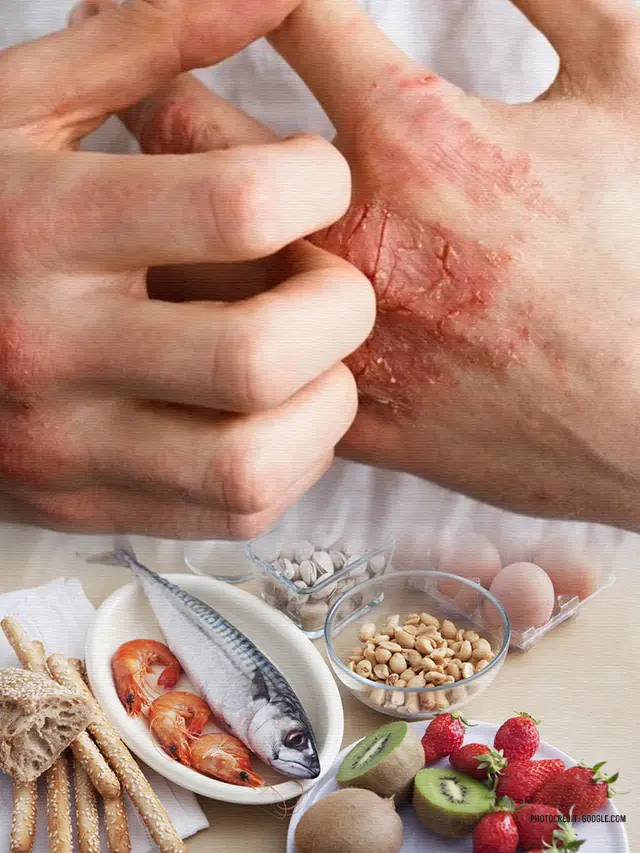
Foods to Avoid if You Have Eczema:
If you have eczema, it may be beneficial to avoid certain foods that are known to trigger or exacerbate symptoms. These foods include.
Cow’s Milk: Dairy products, such as milk, cheese, and yogurt, are frequent triggers for eczema flare-ups, especially in young children.
Eggs: Eggs, particularly the egg whites, can be problematic for individuals with eczema, leading to itching and inflammation.
Peanuts: Peanuts and peanut products are common allergens that can worsen eczema symptoms in susceptible individuals.
Tree Nuts: Tree nuts like almonds, walnuts, and cashews can trigger eczema flare-ups in some people with allergies.
Wheat: Wheat products, including bread, pasta, and cereals, may exacerbate eczema symptoms, possibly due to gluten intolerance or sensitivity.
Soy: Soy and soy-based products are known allergens that can contribute to eczema outbreaks in certain individuals.
Fish and Shellfish: Seafood, such as fish and shellfish, can be problematic for some people with eczema due to allergic reactions.
Processed Foods: Processed foods containing artificial additives, preservatives, and flavorings may aggravate eczema symptoms in some individuals.
Citrus Fruits: Citrus fruits like oranges, lemons, and grapefruits are acidic and can potentially trigger eczema flare-ups in sensitive individuals.
Tomatoes: Some individuals with eczema may experience worsened symptoms after consuming tomatoes and tomato-based products. and some other food and dietry products.
Other Potential Triggers:
Shellfish: Shrimp, crab, lobster, and other shellfish can be triggers for some people with eczema.
Citrus Fruits: Oranges, grapefruits, and other citrus fruits may irritate sensitive skin, worsening eczema symptoms.
Grains: Some people with eczema may be sensitive to certain grains like corn or oats.
Spices: Spices like cinnamon, cloves, and curry powder can irritate the skin and exacerbate eczema.
Managing Eczema Through Some Dietary Changes:
Eczema, with its itchy and inflamed skin, can be a frustrating condition. While there’s no one-size-fits-all cure, dietary changes can significantly improve symptoms for some individuals. Here’s a breakdown of two key dietary approaches for managing eczema.
1. Elimination Diet: Unveiling the Culprits:
An elimination diet is a detective game aimed at identifying specific foods that might be triggering your eczema flare-ups. Here’s how it works.
- Planning: Choose a list of commonly linked eczema triggers like dairy, eggs, peanuts, etc., in consultation with a healthcare professional.
- Elimination: Eliminate these suspected trigger foods from your diet for a set period, typically two weeks.
- Food Diary: Keeping a detailed food diary is crucial. Track everything you eat and monitor your eczema symptoms daily.
- Reintroduction: Slowly reintroduce the eliminated foods one at a time, waiting a few days between each reintroduction. This helps pinpoint which food(s) might be causing problems.
- Reactions: Monitor your skin closely after reintroducing each food. If you experience a flare-up, it suggests that particular food might be a trigger.
2. Probiotics: Potential Allies in the Fight:
Probiotics are live bacteria that offer various health benefits, and some research suggests they might play a role in managing eczema. Here’s what we know.
- Gut Health: Probiotics are believed to promote a healthy gut microbiome, potentially reducing inflammation and improving the gut barrier function.
- Modulating Immunity: Probiotics may help modulate the immune system’s response, potentially reducing the inflammation associated with eczema.
- Limited Evidence: While some studies show promise, more research is needed to definitively confirm the benefits of probiotics for eczema.
Probiotics and Eczema: Important Considerations:
Discuss the use of probiotics with your doctor or dermatologist. Probiotics come in various strains, and the best strain for eczema may vary. Probiotics are generally safe, but side effects like bloating or gas can occur initially.
3.Beyond Diet: A Multifaceted Approach:
While dietary changes can be helpful, managing eczema often requires a multifaceted approach. Here are some additional strategies to consider.
- Moisturizing Regularly: Keeping your skin well-hydrated is crucial for preventing dryness and irritation.
- Avoiding Scratching: Scratching can worsen symptoms. Consider wearing mittens at night to prevent scratching during sleep, especially for children.
- Identifying Environmental Triggers: Dust mites, pet dander, and harsh soaps can trigger flare-ups.
- Stress Management: Stress can exacerbate eczema. Relaxation techniques like yoga or meditation can be beneficial.
Tips for Identifying Food Allergies in Eczema Patients:
Eczema and food allergies, while separate conditions, can often be partners in crime, worsening eczema symptoms for some individuals. Here are some tips to help identify food allergies in eczema patients.
Keep a Food Diary: Encourage eczema patients to keep a detailed food diary to track their dietary intake and any associated eczema flare-ups. This can help identify patterns and potential trigger foods.
Elimination Diet: Consider implementing an elimination diet under the guidance of a healthcare professional. This involves removing common allergenic foods (e.g., dairy, eggs, peanuts, wheat, soy) from the diet for a period of time, typically 2-4 weeks, and then gradually reintroducing them one at a time while monitoring for eczema flare-ups.
Skin Prick Testing: Skin prick testing is a common method used by allergists to identify potential food allergens. A small amount of allergen extract is placed on the skin, and then the skin is pricked or scratched to allow the allergen to enter. If a raised, red bump (wheal) develops, it indicates a positive allergic reaction to that particular allergen.
Blood Tests: Blood tests, such as specific IgE antibody tests, can also be used to identify food allergies by measuring the levels of allergen-specific antibodies in the blood. However, these tests may have limitations and should be interpreted in conjunction with clinical history and other diagnostic methods.
Food Challenge Testing: In some cases, oral food challenge testing may be necessary to confirm or rule out suspected food allergies. This involves gradually introducing small amounts of suspected allergenic foods under medical supervision and monitoring for allergic reactions.
Consider Non-IgE-Mediated Allergies: Keep in mind that not all food allergies involve IgE-mediated reactions. Non-IgE-mediated food allergies, such as food protein-induced enterocolitis syndrome (FPIES) or eosinophilic esophagitis (EoE), may also contribute to eczema symptoms and require specialized diagnostic approaches.
Consulting a Healthcare Professional:
Schedule an appointment: A doctor or dermatologist can offer valuable guidance and conduct tests to identify food allergies.
Discuss your food diary: Sharing your detailed food diary with your doctor can provide crucial insights.
Consider allergy testing: Skin prick tests or blood tests can help identify potential food allergies.
Lifestyle Modifications to Support Eczema Management:
Eczema can be a frustrating itch, but there are ways to manage it beyond just food! Here are some simple lifestyle changes that can work alongside your diet to calm your eczema and improve your quality of life.
Moisture is Your BFF:
Hydrate from the inside out: Drink plenty of water throughout the day to keep your skin hydrated from within.
Moisturize regularly: Use a fragrance-free moisturizer daily to lock in moisture and prevent dry, itchy skin. Look for thicker ointments for extra protection.
Short, cool showers: Hot water can strip away natural oils. Opt for lukewarm showers and pat your skin dry instead of rubbing.
Be Gentle on Your Skin:
Say no to scratchy clothes: Choose soft, loose-fitting clothes made from natural fibers like cotton. Tight clothes can irritate your skin.
Beware of harsh soaps: Skip harsh soaps and detergents that can dry out your skin. Opt for gentle, fragrance-free cleansers.
Identify environmental triggers: Dust mites, pet dander, and harsh soaps can worsen eczema. Try using dust mite covers for pillows and mattresses, and wash bedding regularly. If you have pets, keep them off furniture you use often.
Stress Less, Eczema Less:
Find your calm: Stress can worsen eczema. Try relaxation techniques like yoga, meditation, or deep breathing exercises to manage stress.
Get enough sleep: When you’re well-rested, your body is better equipped to manage inflammation, which can help with eczema.
Maintain a Healthy Diet: Eat a balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats. Incorporate foods that have anti-inflammatory properties, such as fatty fish (salmon, mackerel), flaxseeds, chia seeds, walnuts, and leafy greens. Limit intake of processed foods, sugary snacks, and alcohol, as these can potentially trigger inflammation and worsen eczema symptoms.
Take Proper Treatment: Adhere to the treatment plan prescribed by your healthcare provider, including medications (e.g., topical corticosteroids, antihistamines) and other therapies (e.g., phototherapy, wet wrap therapy). Communicate any concerns or changes in symptoms with your healthcare provider to adjust the treatment plan as needed.
FAQs about Eczema and Food Allergies:
A1: Yes, for some people, certain foods can trigger eczema flare-ups. This is more common in children with eczema.
A2: Certain foods are known to trigger eczema flare-ups, including eggs, dairy, soy, citrus fruits, tomatoes, gluten-containing products, and even certain spices like cloves, cinnamon, and vanilla. Additionally, for individuals with dyshidrotic eczema affecting the hands and feet, foods containing nickel may worsen symptoms.
A3: Keep a food diary to track what you eat and any eczema symptoms. Talk to your doctor about allergy testing or a supervised elimination diet.
A4: Moisturize regularly, avoid scratching, identify and avoid environmental triggers (dust mites, harsh soaps), manage stress, and get enough sleep.
A5: Yes! A doctor or dermatologist can help diagnose eczema, identify triggers (food or environmental), and create a personalized treatment plan.
-Please remember, to always consult with healthcare professionals or Doctors for personalised advice related to medical conditions.
Conclusion:
In conclusion, the connection between eczema and food allergies represents a significant area of interest in understanding and managing this chronic skin condition. While not all individuals with eczema have food allergies, and vice versa, there is substantial overlap between the two conditions, with certain foods known to trigger or exacerbate eczema symptoms in susceptible individuals.





hello sir.