
HEALTH BLOG
Pancreatic Cancer: Symptoms, Treatment, and Chemotherapy
-
Rahul Priydarss
Explore the comprehensive guide to pancreatic cancer, covering symptoms, treatments like chemotherapy, the importance of awareness, causes, diagnosis, stages, and nutritional considerations. Learn how early detection impacts prognosis and access patient stories for inspiration and insight into managing this challenging disease.
Introduction to Pancreatic Cancer:
Pancreatic cancer is a formidable adversary in the realm of oncology, presenting a significant challenge to both patients and healthcare professionals alike. This malignancy originates in the pancreas, a vital organ nestled deep within the abdomen. The pancreas serves dual roles, contributing to both the digestive process and the regulation of blood sugar levels through hormone secretion.
The insidious nature of pancreatic cancer lies in its propensity to remain asymptomatic in its early stages, often eluding detection until it has progressed to an advanced state. When they do arise, symptoms can be vague and nonspecific, further complicating timely diagnosis and intervention.
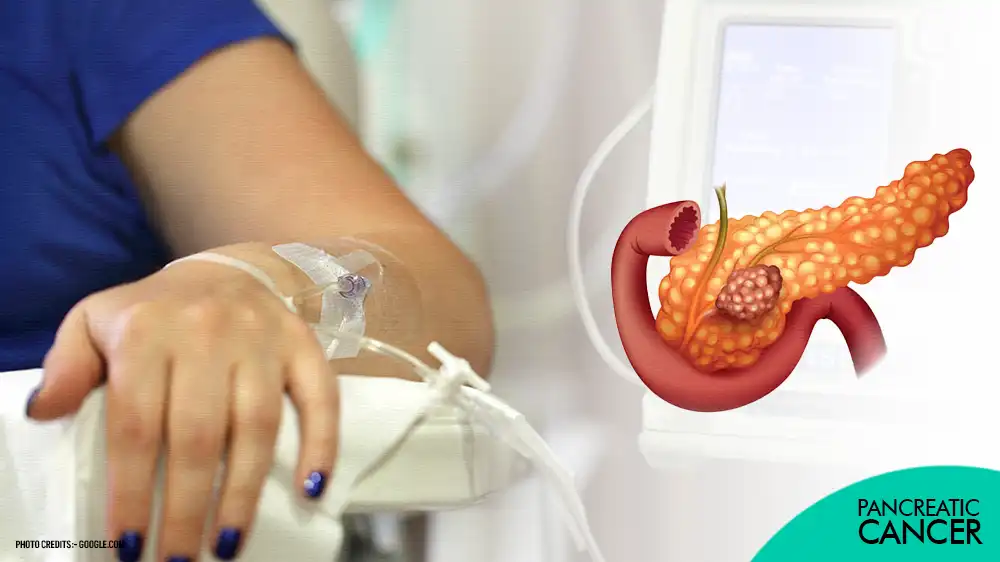
Table of Contents
What is Pancreatic Cancer:
Pancreatic cancer is a type of cancer that starts in the pancreas. The pancreas is a gland shaped like a flat pear located behind your stomach and in front of your spine. It makes digestive juices that help break down food in your small intestine, and hormones that help regulate blood sugar levels.
Pancreatic cancer occurs when cells in your pancreas grow and divide in an uncontrolled way and form a tumor. There are two main types of pancreatic cancer: exocrine and neuroendocrine. Exocrine pancreatic cancer is the most common type. It starts in the cells that make digestive enzymes.
Importance of Awareness and Early Detection of Pancreatic Cancer:
Pancreatic cancer presents a formidable challenge due to its aggressive nature and often asymptomatic early stages. Heightened awareness and early detection play pivotal roles in addressing this disease for several compelling reasons.
1. Improved Prognosis: Early detection of pancreatic cancer significantly improves prognosis and treatment outcomes. When diagnosed at an early stage, the cancer is more likely to be localized and amenable to curative treatment options such as surgery, leading to better chances of long-term survival.
2. Enhanced Treatment Options: Timely diagnosis allows for a wider range of treatment options. Patients diagnosed at an early stage may have access to less invasive therapies, including surgery and targeted therapies, which can be more effective in controlling the disease and preserving quality of life.
3. Better Quality of Life: Early detection improves survival rates and enhances patients’ overall quality of life. By identifying the disease before it has advanced, individuals may experience fewer symptoms and complications, allowing them to maintain their daily activities and enjoy a higher quality of life during treatment.
4. Reduced Healthcare Costs: Detecting pancreatic cancer early can lead to reduced healthcare costs. Early-stage treatment is often less intensive and may require fewer resources than advanced-stage interventions, resulting in lower medical expenses for patients and healthcare systems.
5. Empowerment through Education: Increasing awareness about pancreatic cancer symptoms, risk factors, and screening methods empowers individuals to take proactive steps in managing their health. Educated patients are more likely to recognize potential warning signs, seek timely medical attention, and engage in preventive measures to reduce their risk of developing the disease.
6. Support for Research and Innovation: Heightened awareness of pancreatic cancer fosters support for research initiatives aimed at improving early detection methods, developing novel treatment modalities, and unraveling the underlying mechanisms of the disease. Increased funding and public interest in pancreatic cancer research can accelerate progress toward finding effective solutions.
Causes of Pancreatic Cancer:
The causes of pancreatic cancer are multifactorial, involving a combination of genetic, environmental, and lifestyle factors. While the exact cause of pancreatic cancer remains elusive, several risk factors have been identified.
Smoking: Tobacco use, including cigarette smoking, is one of the most significant risk factors for pancreatic cancer. Smokers are at a considerably higher risk of developing the disease compared to non-smokers.
Age: Advancing age is a major risk factor for pancreatic cancer, with the majority of cases diagnosed in individuals over the age of 65. The risk increases with age, with the highest incidence seen in those over 80 years old.
Family History and Genetics: A family history of pancreatic cancer or certain inherited genetic syndromes can elevate the risk of developing the disease. Mutations in genes such as BRCA1, BRCA2, PALB2, and Lynch syndrome genes (MLH1, MSH2, MSH6, PMS2) have been linked to an increased risk of pancreatic cancer.
Chronic Pancreatitis: Chronic inflammation of the pancreas, known as chronic pancreatitis, is associated with an increased risk of developing pancreatic cancer. Long-standing inflammation can lead to changes in pancreatic cells that promote cancer development.
Obesity and Poor Diet: Obesity, as well as a diet high in red and processed meats, saturated fats, and low in fruits and vegetables, has been linked to a higher risk of pancreatic cancer. Conversely, a diet rich in fruits, vegetables, and whole grains may help reduce the risk.
Diabetes: Chronic diabetes, particularly type 2 diabetes, is associated with an increased risk of pancreatic cancer. However, the relationship between diabetes and pancreatic cancer is complex and not fully understood.
Alcohol Consumption: Heavy alcohol consumption over a prolonged period is a known risk factor for pancreatic cancer. Alcohol abuse can contribute to chronic pancreatitis, which in turn increases the risk of developing pancreatic cancer.
Exposure to Certain Chemicals: Occupational exposure to certain chemicals, such as benzene and certain pesticides, has been linked to an increased risk of pancreatic cancer.
Symptoms of Pancreatic Cancer:
Pancreatic cancer often does not cause noticeable symptoms in its early stages, making it challenging to detect. However, as the cancer progresses, various symptoms may manifest. These symptoms can include:
Abdominal Pain: Persistent pain in the abdomen or back, often located in the upper abdomen or mid-back region, is a common symptom of pancreatic cancer. This pain may worsen after eating or lying down and may be accompanied by nausea.
Jaundice: Yellowing of the skin and whites of the eyes, known as jaundice, can occur when pancreatic cancer obstructs the bile duct. This obstruction prevents bile from flowing properly and causes a buildup of bilirubin in the bloodstream, resulting in jaundice. Other symptoms of jaundice may include dark urine, pale-colored stools, and itching.
Unintended Weight Loss: Significant and unexplained weight loss is often a symptom of pancreatic cancer. This weight loss may occur even if the person has not made any changes to their diet or exercise routine.
Loss of Appetite: Pancreatic cancer can cause a decreased appetite, leading to a reduced intake of food and subsequent weight loss.
Digestive Problems: Digestive issues such as nausea, vomiting, diarrhea, or changes in bowel habits may occur as a result of pancreatic cancer affecting the digestive system.
New-Onset Diabetes: In some cases, pancreatic cancer may cause new-onset diabetes or exacerbate existing diabetes. This occurs when the cancer affects the pancreas’s ability to produce insulin, leading to elevated blood sugar levels.
Fatigue: Generalized fatigue and weakness may be experienced due to the body’s response to cancer or as a result of nutritional deficiencies caused by pancreatic cancer.
Diagnosis of Pancreatic Cancer:
Diagnosing pancreatic cancer typically involves a combination of medical history assessment, physical examination, imaging tests, and laboratory tests. The process may include the following steps.
Medical History and Physical Examination: The healthcare provider will review the patient’s medical history and inquire about any symptoms they may be experiencing. A physical examination may also be conducted to check for signs of pancreatic cancer, such as jaundice or abdominal tenderness.
Imaging Tests: Imaging tests are crucial for visualizing the pancreas and detecting any abnormalities. Common imaging techniques used in the diagnosis of pancreatic cancer include.
- CT Scan (Computed Tomography): A CT scan uses X-rays to create detailed cross-sectional images of the pancreas and surrounding organs.
- PET scan: A PET scan uses a radioactive tracer to create images of your body. Cancer cells are more metabolically active than healthy cells and take up more tracer, appearing brighter on the scan. A PET scan is often combined with a CT scan (PET-CT scan) to provide both anatomical and functional information.
- MRI (Magnetic Resonance Imaging): MRI uses magnetic fields and radio waves to produce detailed images of the pancreas and nearby structures.
- Endoscopic Ultrasound (EUS): EUS involves inserting a thin, flexible tube with an ultrasound probe into the stomach to obtain high-resolution images of the pancreas and surrounding tissues.
- Endoscopic Retrograde Cholangiopancreatography (ERCP): ERCP combines endoscopy with X-ray imaging to examine the pancreatic and bile ducts for blockages or abnormalities.
Biopsy: A biopsy is the only definitive way to diagnose pancreatic cancer. During a biopsy, a small sample of tissue is removed from the pancreas and examined under a microscope by a pathologist to look for cancerous cells. There are several ways to obtain a tissue sample for pancreatic cancer biopsy, including.
- Fine-needle aspiration (FNA): This is a minimally invasive procedure that uses a thin needle to withdraw a small sample of tissue from the pancreas. FNA is often performed with the guidance of ultrasound or CT scan.
- Needle core biopsy: This procedure uses a slightly larger needle to remove a core of tissue from the pancreas. Needle core biopsy may also be done with ultrasound or CT scan guidance.
- Surgical biopsy: In some cases, a surgical procedure may be needed to obtain a tissue sample for biopsy. This may be done laparoscopically (using small incisions and a camera) or through an open surgical incision.
Blood Tests: Blood tests may be conducted to assess various markers associated with pancreatic cancer, such as levels of certain enzymes (e.g., CA 19-9) or substances released by cancer cells.
Laparoscopy: In some cases, laparoscopic surgery may be performed to obtain a direct visual inspection of the pancreas and surrounding tissues. This procedure may help determine the extent of the cancer and whether it has spread to nearby organs or tissues.
Stages of Pancreatic Cancer:
Doctors use a staging system to classify pancreatic cancer based on the size of the tumor and whether it has spread to other parts of the body. The most common staging system is the American Joint Committee on Cancer (AJCC) TNM staging system. Here’s a breakdown of what the TNM system represents and how it’s used for pancreatic cancer staging.
- T: This category refers to the size and extent of the primary tumor in the pancreas. It ranges from TX (primary tumor cannot be assessed) to T4 (tumor has grown into nearby major blood vessels or organs).
- N: This category indicates whether the cancer has spread to lymph nodes. N0 means no lymph node involvement, while higher N stages indicate progressive spread to lymph nodes in the region.
- M: This category signifies whether the cancer has metastasized (spread) to distant organs beyond the pancreas and nearby lymph nodes. M0 indicates no distant spread, while M1 signifies metastasis.
Stage Groups: Based on the TNM classification, pancreatic cancer is assigned to different stages. Here’s a general overview of the stages:
- Stage 0 (Carcinoma in situ): This is the earliest stage of pancreatic cancer. The abnormal cells are still confined to the top layer of the pancreatic ducts and haven’t invaded deeper tissues. (Tis, N0, M0)
- Stage IA: The tumor is 2 centimeters or smaller and has not spread to lymph nodes or other parts of the body. (T1, N0, M0)
- Stage IB: The tumor is larger than 2 centimeters but not more than 4 centimeters and has not spread to lymph nodes or other parts of the body. (T2, N0, M0)
- Stage IIA: The tumor is larger than 4 centimeters and extends beyond the pancreas but has not spread to nearby arteries, veins, lymph nodes, or other parts of the body. (T3, N0, M0)
- Stage IIB: The tumor can be any size but has not spread to nearby arteries or veins, although lymph node involvement may be present. (T any, N1, M0)
- Stage III: The cancer has spread to nearby major blood vessels or nerves but has not metastasized to distant organs. (T any, N2, M0)
- Stage IV: The cancer has spread to distant organs such as the liver, lungs, or bones. (T any, N any, M1)
Treatment Options for Pancreatic Cancer:
Treatment options for pancreatic cancer depend on several factors, including the stage of the cancer, the location of the tumor, the patient’s overall health, and personal preferences. The main treatment modalities for pancreatic cancer include.
Surgery:
Surgical resection is often the preferred treatment for pancreatic cancer if the tumor is localized and has not spread beyond the pancreas. The type of surgery performed depends on the location and size of the tumor. Common surgical procedures for pancreatic cancer include.
- Whipple Procedure (Pancreaticoduodenectomy): This surgery involves removing the head of the pancreas, part of the small intestine, the gallbladder, the bile duct, and sometimes a portion of the stomach.
- Distal Pancreatectomy: In this procedure, the tail and body of the pancreas are removed, often along with the spleen.
- Total Pancreatectomy: This surgery involves removing the entire pancreas, as well as the gallbladder, spleen, part of the stomach, and surrounding lymph nodes.
Chemotherapy:
Chemotherapy is a common treatment option for pancreatic cancer, often used in combination with surgery, radiation therapy, or as a standalone treatment for advanced or metastatic disease. Chemotherapy involves the use of powerful drugs to kill cancer cells or slow their growth by interfering with their ability to divide and multiply.
Chemotherapy Administration Ways:
- Neoadjuvant Chemotherapy: Neoadjuvant chemotherapy is given before surgery to shrink the tumor and make it more manageable for surgical removal. This approach may help improve the chances of successful surgery and reduce the risk of cancer recurrence.
- Adjuvant Chemotherapy: Adjuvant chemotherapy is given after surgery to eliminate any remaining cancer cells and reduce the risk of cancer recurrence. It aims to improve long-term outcomes by targeting residual cancer cells that may not have been removed during surgery.
- Palliative Chemotherapy: For patients with advanced or metastatic pancreatic cancer who are not candidates for surgery, palliative chemotherapy may be used to help relieve symptoms, control the growth of the tumor, and improve quality of life. Palliative chemotherapy may also be used to prolong survival in some cases.
Chemotherapy drugs:
- Gemcitabine: Gemcitabine is a chemotherapy drug that is often used as a first-line treatment for pancreatic cancer, either alone or in combination with other drugs. It works by interfering with the synthesis of DNA and RNA, thereby preventing cancer cells from dividing and multiplying.
- Fluorouracil (5-FU): Fluorouracil is another chemotherapy drug commonly used to treat pancreatic cancer. It works by inhibiting the enzyme thymidylate synthase, which is necessary for DNA synthesis in cancer cells.
- Paclitaxel: Paclitaxel is a chemotherapy drug that works by disrupting the normal function of microtubules, structures within the cell that are essential for cell division and growth.
- Nab-paclitaxel: Nab-paclitaxel is a newer formulation of paclitaxel that is bound to albumin, a protein found in blood. This formulation allows for higher concentrations of the drug to be delivered to the tumor site.
- Oxaliplatin, and Irinotecan: These drugs are sometimes used in combination with other chemotherapy agents for the treatment of advanced pancreatic cancer.
Radiation Therapy:
Radiation therapy uses high-energy beams to target and destroy cancer cells. It may be used alone or in combination with chemotherapy before or after surgery to improve local control of the tumor or relieve symptoms in advanced cases.
Targeted Therapy:
Targeted therapies are drugs that specifically target certain molecular pathways involved in cancer growth and progression. Examples of targeted therapies used for pancreatic cancer include erlotinib (Tarceva) and cetuximab (Erbitux), which target the epidermal growth factor receptor (EGFR), and sunitinib (Sutent) and pazopanib (Votrient), which target vascular endothelial growth factor (VEGF) receptors.
Immunotherapy:
Immunotherapy drugs, such as pembrolizumab (Keytruda) and nivolumab (Opdivo), work by harnessing the body’s immune system to target and attack cancer cells. While immunotherapy has shown promise in certain cancers, its role in pancreatic cancer treatment is still being studied in clinical trials.
Palliative Care:
Palliative care focuses on improving the quality of life for patients with advanced pancreatic cancer by managing symptoms such as pain, nausea, and fatigue. Palliative care may involve medications, radiation therapy, nutritional support, and psychosocial interventions.
Nutrition Need in Pancreatic Cancer:
Nutrition plays a crucial role in managing pancreatic cancer, as it can help support the body’s immune system, maintain strength and energy levels, and improve overall quality of life. However, pancreatic cancer and its treatments can often lead to challenges with eating and digestion. Here are some important considerations for nutrition in pancreatic cancer.
Maintain Adequate Caloric Intake: Pancreatic cancer and its treatments can lead to weight loss and malnutrition. It’s essential to consume enough calories to maintain a healthy weight and prevent muscle wasting. Eating small, frequent meals and snacks throughout the day can help increase calorie intake.
Focus on Nutrient-Dense Foods: Choose nutrient-dense foods that provide essential vitamins, minerals, and antioxidants to support overall health and immunity. Examples include fruits, vegetables, whole grains, lean proteins, and healthy fats.
Include Protein-Rich Foods: Protein is essential for maintaining muscle mass and strength during cancer treatment. Include protein-rich foods such as poultry, fish, eggs, dairy products, beans, lentils, tofu, and nuts in your diet.
Stay Hydrated: Adequate hydration is important for managing side effects such as nausea, vomiting, and diarrhea, which are common in pancreatic cancer. Drink plenty of fluids throughout the day, including water, herbal teas, broth-based soups, and electrolyte-rich beverages.
Manage Digestive Symptoms: Pancreatic cancer and its treatments can affect digestion and lead to symptoms such as nausea, vomiting, diarrhea, and abdominal pain. Work with a healthcare provider or dietitian to develop strategies to manage these symptoms, such as dietary modifications, medications, and lifestyle changes.
Consider Pancreatic Enzyme Replacement Therapy (PERT): For individuals with pancreatic cancer who experience pancreatic enzyme insufficiency, PERT may be prescribed to aid digestion. PERT supplements contain enzymes that help break down fats, proteins, and carbohydrates, improving nutrient absorption and reducing symptoms such as diarrhea and steatorrhea (fatty stools).
Limit High-Fat Foods: High-fat foods can be difficult to digest, especially for individuals with pancreatic cancer or those who have undergone surgery to remove part of the pancreas. Limit intake of fried foods, fatty meats, full-fat dairy products, and rich desserts.
Monitor Blood Sugar Levels: Pancreatic cancer and its treatments can affect blood sugar levels, especially in individuals with pre-existing diabetes. Monitor blood sugar levels regularly and consume balanced meals and snacks to help regulate blood sugar levels.
Seek Support from a Registered Dietitian: A registered dietitian can provide personalized nutrition counseling and support for individuals with pancreatic cancer. They can help develop a tailored nutrition plan to meet individual needs, manage symptoms, and optimize nutritional status during treatment.
Patient Stories and Testimonials:
Reading about the experiences of others with pancreatic cancer can be a source of inspiration and knowledge. Here are some resources where you can find patient stories and testimonials.
Pancreatic Cancer Action Network: This organization has a section dedicated to “Survivor Stories” featuring patients who are living with or beyond pancreatic cancer https://pancan.org/stories/survivors/.
Patient Stories on Hospital Websites: Many cancer treatment centers share patient stories on their websites. You can find these by searching for “[Hospital Name] Pancreatic Cancer Patient Stories”. Here are a few examples:
UPMC Hillman Cancer Center https://hillman.upmc.com/cancer-care/pancreatic/patient-stories
Columbia University Department of Surgery https://pancan.org/stories/survivors/
City of Hope https://www.cancer.org/cancer/latest-news/stories-of-hope.html
Pancreatic Cancer UK: This UK-based organization also features real-life stories from patients https://www.pancreaticcancer.org.uk/real-life-stories-section/.
FAQs about Pancreatic Cancer:
A1: No, chemotherapy is one option. Surgery, radiation, and targeted therapies are also used depending on the stage and type of cancer.
A2: Gemcitabine, nab-paclitaxel, fluorouracil (5-FU), irinotecan, and oxaliplatin are some of the most common drugs used in various combinations.
A3: Chemo is usually given in cycles with breaks in between for recovery. The drugs can be administered intravenously or orally.
A4: Fatigue, nausea, vomiting, hair loss, and mouth sores are common side effects. Your doctor can advise on managing these.
A5: Yes, research is ongoing. Immunotherapy and targeted therapies are being explored alongside traditional chemotherapy for potentially better outcomes.
-Please remember, to always consult with healthcare professionals or Doctors for personalised advice related to medical conditions.
Conclusion:
In conclusion, Pancreatic Cancer poses a significant challenge due to its aggressive nature and often asymptomatic early stages. Awareness, early detection, and access to comprehensive treatment options are crucial in addressing this formidable disease. By understanding its symptoms, risk factors, and diagnostic methods, individuals can take proactive steps to manage their health effectively. Additionally, ongoing research and support for innovative treatments are essential in advancing the fight against pancreatic cancer. Through collective efforts, we can improve outcomes, enhance quality of life, and strive for better outcomes for those affected by this disease.




